Ati n200 final exam day (mental health & med Surg) exam
Total Questions : 92
Showing 25 questions, Sign in for moreA client has been diagnosed with tuberculosis and is receiving isoniazid. What information should the nurse incorporate into the client's teaching plan?
Explanation
Choice A reason:
Isoniazid, an antitubercular medication, can cause peripheral neuropathy, a form of nerve damage characterized by numbness, tingling, or pain, particularly in the hands and feet. This side effect is due to the drug's interference with the normal metabolism of vitamin B6 (pyridoxine). Supplementation with vitamin B6 is recommended to prevent this complication. The normal daily recommended intake for vitamin B6 in adults ranges from 1.3 to 1.7 mg.
Choice B reason:
While it is true that isoniazid can cause discoloration of bodily fluids, turning urine and tears orange, this is not a harmful side effect and does not require intervention. It is, however, important to inform the client of this possibility to prevent alarm.
Choice C reason:
There is no evidence to suggest that routine hearing exams are necessary for clients taking isoniazid unless they have pre-existing hearing conditions or are taking other medications known to affect hearing. Therefore, this is not a standard part of the teaching plan for clients on isoniazid.
Choice D reason:
Photosensitivity reactions are not commonly associated with isoniazid use. While wearing sunscreen is generally good advice for skin protection, it is not specifically related to the administration of isoniazid and thus would not be the primary information to include in the teaching plan.
A nurse is caring for a client who has just arrived in the postoperative unit after undergoing a laminectomy and spinal fusion. What action should the nurse take?
Explanation
Choice A reason:
Assisting the client to turn by having them grasp the side rails is not recommended immediately following a laminectomy and spinal fusion. This action could place undue stress on the surgical site and potentially disrupt the healing process. Postoperative care typically involves minimizing movement of the spine to prevent complications.
Choice B reason:
Maintaining strict bedrest for 48 hours postoperatively is not a current standard of care following a laminectomy and spinal fusion. Early ambulation, as tolerated, is encouraged to promote circulation and prevent complications such as deep vein thrombosis (DVT) and pulmonary embolism (PE).
Choice C reason:
Assessing the client's pain level and administering pain medication as needed is a critical nursing intervention postoperatively. Effective pain management is essential for promoting patient comfort, facilitating early mobilization, and preventing complications. Pain assessment and management should be tailored to the individual's needs and carried out with regular monitoring.
Choice D reason:
Placing the client in the prone position is not typically advised following a laminectomy and spinal fusion, as it may put pressure on the surgical site and cause discomfort. The preferred position is usually on the back or occasionally on the side with proper support, depending on the surgeon's protocol and the client's comfort.
A nurse is caring for a client with a diagnosis of left lower lobe pneumonia who experiences pain when coughing. What intervention should the nurse include in the care plan?
Explanation
Choice A reason:
Limiting ambulation is not typically recommended as part of the management for pneumonia. While rest is important, some movement is beneficial for preventing complications such as deep vein thrombosis. Ambulation should be encouraged as tolerated to promote circulation and prevent stasis of secretions.
Choice B reason:
Administering pain medication every two hours may not be necessary and could lead to overmedication. Pain management should be based on the client's reported pain levels and response to medication, with adjustments made as needed for effective relief.
Choice C reason:
Encouraging the client to hold their chest with a pillow or hands, known as splinting, can help reduce the pain experienced during coughing by providing support and stabilizing the chest wall. This technique is a non-pharmacological intervention that can effectively manage pain associated with coughing in pneumonia patients.
Choice D reason:
Teaching pursed-lip breathing and deep breathing techniques is beneficial for clients with respiratory conditions, including pneumonia. These techniques can help improve ventilation and oxygenation, but they are not specifically aimed at managing pain during coughing. However, they can be included as part of the overall respiratory care plan.
A nurse is talking to a client who is worried about developing gout. Which of the following factors should the nurse recognize as risk factors for this condition? (Select all that apply)
Explanation
Choice A reason:
Obesity is a significant risk factor for gout. It can lead to increased production and decreased excretion of uric acid, which in turn can cause gout attacks. The normal body mass index (BMI) range is 18.5 to 24.9, and a BMI of 30 or above is considered obese.
Choice B reason:
Regular consumption of beer can increase the risk of gout. Beer is high in purines, which the body breaks down into uric acid, and alcohol can reduce the excretion of uric acid by the kidneys. Moderation in alcohol consumption is advised, with the recommendation being up to one drink per day for women and up to two drinks per day for men.
Choice C reason:
Thiazide diuretics are associated with an increased risk of gout. They can decrease the kidney's ability to remove uric acid from the body, leading to its accumulation. When prescribing thiazide diuretics, healthcare providers often monitor uric acid levels and consider alternative medications if the patient has a history of gout.
Choice D reason:
Depression is not directly identified as a risk factor for developing gout. However, some lifestyle factors associated with depression, such as poor diet and inactivity, could indirectly increase the risk.
Choice E reason:
Hypertension is a known risk factor for gout. High blood pressure can impair kidney function, which is responsible for excreting uric acid, thus leading to hyperuricemia and gout. The normal range for blood pressure is considered to be below 120/80 mmHg.
A nurse is caring for a client diagnosed with deep vein thrombosis who suddenly reports severe chest pain, shortness of breath, and extreme anxiety. The nurse suspects the client may have developed a pulmonary embolism. What intervention should the nurse perform first?
Explanation
Choice A reason:
Performing a 12-lead electrocardiogram and calling a rapid response team are important steps when a pulmonary embolism is suspected. However, these actions are not the immediate first-line interventions. The priority is to address the client's oxygenation needs to prevent further hypoxemia and potential cardiac arrest.
Choice B reason:
Elevating the head of the bed and applying 2 liters of nasal oxygen is the most appropriate initial intervention. This position helps improve the expansion of the lungs and oxygenation, while the supplemental oxygen can help alleviate hypoxemia, which is critical in the management of a pulmonary embolism.
Choice C reason:
While ensuring the client remains calm is beneficial, administering lorazepam is not the first-line treatment for a suspected pulmonary embolism. Lorazepam may be used for its anxiolytic effects, but it does not address the immediate life-threatening issues of oxygenation and potential hemodynamic instability.
Choice D reason:
Increasing the intravenous rate may be considered to maintain adequate hydration and venous return, but it is not the first intervention for a suspected pulmonary embolism. The priority is to stabilize the client's respiratory status and oxygenation.
After successfully losing one pound per week for several months, an obese client at the clinic has not experienced any weight loss in the past month. What should the nurse do first?
Explanation
Choice A reason:
Reviewing the diet and exercise guidelines with the client is an important step, but it may not address the immediate issue of the weight loss plateau. It's essential to first understand if the client has adhered to the guidelines before reviewing them.
Choice B reason:
Asking the client about any changes in diet or exercise patterns is the first step in identifying potential causes for the weight loss plateau. Changes in lifestyle, stress levels, eating habits, or physical activity can all contribute to a halt in weight loss. Understanding these factors can help the nurse tailor further advice and support.
Choice C reason:
Recommending a further reduction in calorie intake might not be the best initial approach. It's important to ensure that the client is not already consuming too few calories, which can slow metabolism and hinder weight loss. Moreover, drastic calorie reduction can be unsustainable and lead to nutritional deficiencies.
Choice D reason:
Instructing the client to record weights weekly is a useful tool for monitoring progress, but it does not address the current issue of the weight loss plateau. It's a supportive action that should follow after understanding and addressing the reasons behind the plateau.
A client with Type 2 diabetes, managed with diet and metformin, also has chronic obstructive pulmonary disease (COPD). During a COPD exacerbation, the client is prescribed prednisone to manage inflammation. Which side effect should the nurse monitor in this client?
Explanation
Choice A reason:
Prednisone is a corticosteroid that can cause hyperglycemia, especially in clients with diabetes. The nurse should monitor blood glucose levels because prednisone can increase insulin resistance and hepatic glucose production, leading to elevated blood glucose levels. Normal fasting blood glucose levels range from 70 to 99 mg/dL, and for individuals with diabetes, maintaining blood glucose levels within the target range set by their healthcare provider is crucial to prevent complications.
Choice B reason:
While corticosteroids can affect electrolyte balance, they typically cause a decrease in potassium levels, not an increase. Therefore, monitoring for hypokalemia, rather than hyperkalemia, would be more appropriate when a patient is on prednisone. The normal range for serum potassium is 3.5 to 5.0 mEq/L.
Choice C reason:
Corticosteroids like prednisone can cause leukocytosis, an increase in white blood cell count, as part of their immunosuppressive action. However, this is generally not a harmful side effect unless accompanied by infection or other complications. The normal range for white blood cell count is approximately 4,500 to 11,000 cells per microliter.
Choice D reason:
Increased ketones in the urine, or ketonuria, is not a typical side effect of prednisone. Ketonuria is more commonly associated with uncontrolled diabetes, particularly Type 1 diabetes, when there is an insulin deficiency and the body resorts to fat breakdown, leading to ketone production.
A nurse is caring for a client diagnosed with an acute exacerbation of chronic obstructive pulmonary disease (COPD). The client's assessment shows a respiratory rate of 28/min, SpO2 at 90%, and reports of mild dyspnea and anxiety while at rest. What should the nurse include in the client's discharge teaching plan?
Explanation
Choice A reason:
Using bronchodilators every 2 hours as needed may not be appropriate for all clients. Bronchodilators are typically used on a schedule or as needed based on symptoms, but overuse can lead to tolerance and decreased effectiveness. The nurse should provide education on the proper use and timing of bronchodilators.
Choice B reason:
Pursed-lip breathing is a technique that helps control shortness of breath and improve ventilation. It can slow down the client's breathing, promote relaxation, and ensure more effective lung function. This technique is particularly beneficial during an acute exacerbation of COPD and should be included in the discharge teaching plan.
Choice C reason:
Increasing home oxygen without proper assessment can be dangerous. Oxygen therapy should be titrated based on the client's oxygen saturation and clinical status. Clients with COPD are at risk of CO2 retention, and too much oxygen can suppress their drive to breathe. The nurse should educate the client on monitoring their SpO2 and when to adjust oxygen levels, typically under the guidance of a healthcare provider.
Choice D reason:
Huff coughing is a technique used to clear mucus from the airways. While it can be effective, it should be taught by a respiratory therapist or nurse who can assess the client's ability to perform the technique correctly. It is not the first-line teaching for a client being discharged with an acute exacerbation of COPD.
A client diagnosed with schizophrenia functions well while hospitalized but deteriorates after being discharged. What does the therapeutic milieu offer that might be lacking in the home environment?
Explanation
Choice A reason:
Mandated activities are part of a therapeutic milieu, but they are not the primary element that contributes to the stability of a client with schizophrenia. While these activities provide a routine, they do not encompass the comprehensive support system that structured programming offers.
Choice B reason:
Visitor restrictions can be a component of a therapeutic milieu, particularly in inpatient settings, to ensure a safe and controlled environment. However, this is not typically what is missing in the home environment that leads to decompensation.
Choice C reason:
Structured programming is a key element of the therapeutic milieu that provides a stable and predictable environment, which is often lacking at home. This structure includes scheduled therapy sessions, social interactions, and activities that are designed to improve coping skills and social functioning. The consistency and predictability of structured programming can significantly benefit individuals with schizophrenia, helping them maintain functional stability.
Choice D reason:
Peer pressure is not a therapeutic aspect of the milieu. In fact, peer pressure can sometimes be negative. However, positive peer interactions and support are important in a therapeutic setting, as they can provide encouragement and a sense of community.
A client who has been a victim of intimate partner abuse is experiencing anxiety and crying. What action should the nurse take?
Explanation
Choice A reason:
Allowing the client some time alone could be beneficial in certain situations where the client prefers solitude to process their emotions. However, in the context of intimate partner abuse, leaving the client alone when they are visibly distressed may not provide the immediate support and safety they need.
Choice B reason:
Remaining with the client is crucial in providing emotional support and ensuring their safety. Victims of intimate partner abuse often feel isolated and scared; having a compassionate presence can offer comfort and reassurance. The nurse's presence can also help in assessing the client's immediate needs and risks, and in facilitating access to further support and resources.
Choice C reason:
Making an audio recording without the client's consent could be a violation of privacy and trust. It is essential to respect the client's autonomy and confidentiality, especially in sensitive situations involving abuse. The priority should be to address the client's emotional state and safety, not to gather evidence.
Choice D reason:
Encouraging the client to write down their thoughts can be a therapeutic tool and may be suggested as part of ongoing therapy or coping strategies. However, it should not be the first action taken when the client is in acute distress. Immediate emotional support and safety planning are more pressing concerns.
A nurse carries out a care plan for a client with the issue of Impaired Gas Exchange due to left lower lobe pneumonia. Which findings would indicate that the nursing interventions were effective? (Select all that apply)
Explanation
Choice A reason:
Cyanosis, or a bluish discoloration of the skin, particularly in the nail beds, is a sign of inadequate oxygenation and would not indicate successful intervention. The absence of cyanosis would be a positive outcome, reflecting improved oxygen saturation.
Choice B reason:
Lungs clear to auscultation would indicate that air is moving through all regions of the lungs without obstruction from fluid or mucus, which is a sign of recovery from pneumonia. This finding suggests that the interventions aimed at improving gas exchange, such as positioning, deep breathing exercises, and suctioning if needed, have been effective.
Choice C reason:
The inability to speak in full sentences often indicates respiratory distress and would not be a sign of successful nursing intervention. An improvement would be the client's ability to speak in full sentences without difficulty, reflecting better lung function and gas exchange.
Choice D reason:
Pulse oximetry readings between 94-96% on room air are within normal limits and indicate adequate oxygen saturation and gas exchange. This is a clear sign that the client's respiratory status has improved, and the interventions for Impaired Gas Exchange have been successful.
Choice E reason:
Bronchovesicular breath sounds are normal breath sounds heard over the major bronchi and are typically moderate in pitch and intensity. However, they are not specifically indicative of successful intervention for Impaired Gas Exchange. The absence of abnormal sounds such as crackles or wheezes would be more relevant.
A nurse is caring for a client who has experienced recurrent episodes of cystitis. When considering the potential progression of the infection, which symptoms should the client be instructed to monitor?
Explanation
Choice A reason:
Dysuria, or painful urination, is a common symptom of cystitis and indicates inflammation of the bladder, often caused by a urinary tract infection (UTI). While it is a symptom to monitor, it does not necessarily indicate progression of the infection.
Choice B reason:
An increased frequency of urination can be a symptom of cystitis due to irritation of the bladder lining. However, like dysuria, it is a common symptom of a UTI and may not signify that the infection is worsening.
Choice C reason:
Pyuria, the presence of white blood cells in the urine, and hematuria, the presence of blood in the urine, are both indicators of inflammation and infection. These symptoms can occur with cystitis but are also not specific to the progression of the infection.
Choice D reason:
Fever is a systemic response to infection and can indicate that a UTI, such as cystitis, is worsening or spreading, possibly to the kidneys, which is known as pyelonephritis. Monitoring for fever is important because it may necessitate more aggressive treatment, such as antibiotics, and possibly hospitalization if the infection is severe.
A nurse is assessing a client who has been newly diagnosed with early-onset osteoarthritis. Which manifestation should the nurse anticipate?
Explanation
Choice A reason:
Ulnar deviation, which is the angling of the fingers towards the little finger side of the hand, is more commonly associated with rheumatoid arthritis, not osteoarthritis. Osteoarthritis typically affects the joint's cartilage, leading to pain and stiffness, rather than causing the fingers to deviate.
Choice B reason:
Symmetric joint involvement is also more characteristic of rheumatoid arthritis. Osteoarthritis usually affects joints asymmetrically, meaning it's more likely to affect one side of the body or one particular joint at a time.
Choice C reason:
Weight loss is not a direct manifestation of osteoarthritis. In fact, being overweight is a risk factor for developing osteoarthritis due to the increased stress on weight-bearing joints. However, weight management through diet and exercise can be part of the treatment plan for osteoarthritis to alleviate symptoms and improve joint function.
Choice D reason:
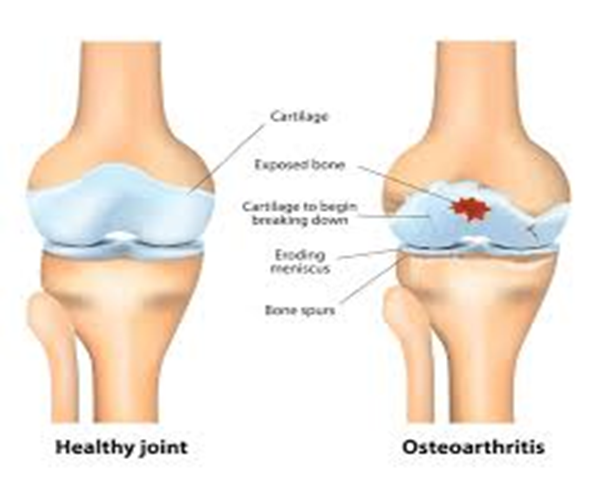
Joint stiffness and limited range of motion are hallmark manifestations of osteoarthritis. These symptoms result from the breakdown of cartilage within the joints, which leads to pain and difficulty moving the affected joint. Stiffness is often most noticeable upon waking or after periods of inactivity, and the range of motion may decrease as the condition progresses.
A client diagnosed with depression has been prescribed duloxetine. Which statement by the client would indicate to the nurse that the medication education has been effective?
Explanation
Choice A reason:
Duloxetine is a medication that should not be stopped abruptly due to the risk of withdrawal symptoms. Gradual tapering is recommended to minimize these symptoms. This understanding by the client indicates effective medication teaching.
Choice B reason:
The statement about the medication being safe with herbal supplements is incorrect. Patients should consult their healthcare provider before using herbal supplements with duloxetine, as there can be interactions.
Choice C reason:
The need to avoid aged cheese is associated with monoamine oxidase inhibitors (MAOIs), not duloxetine, which is a selective serotonin and norepinephrine reuptake inhibitor (SNRI). This statement does not reflect accurate medication teaching for duloxetine.
Choice D reason:
Taking extra doses for anxiety without consulting a healthcare provider is not recommended. Duloxetine dosing should be consistent and as prescribed by a healthcare provider. This statement suggests a misunderstanding of medication management.
A nurse identifies the problem of ineffective airway clearance in a client with pneumonia. Which assessment data most strongly supports this problem?
Explanation
Choice A reason:
A respiratory rate of 24/min is slightly elevated, which can be expected in a client with pneumonia due to the body's attempt to increase oxygen intake and carbon dioxide elimination. However, this rate does not directly indicate ineffective airway clearance.
Choice B reason:
A weak, nonproductive cough is a key indicator of ineffective airway clearance. In pneumonia, the presence of secretions in the airways is common, and an effective cough is necessary to clear these secretions. A weak cough that does not produce sputum suggests that the client is unable to clear their airways effectively, which can lead to impaired gas exchange and worsening of symptoms.
Choice C reason:
Pulse oximetry (SpO2) of 90% indicates that the client's oxygen saturation is below the normal range, which is typically between 95-100% for healthy individuals. While this finding is concerning and warrants intervention, it is a result of ineffective airway clearance rather than a direct indicator of it.
Choice D reason:
Shortness of breath with activity is common in clients with pneumonia and can result from various factors, including impaired gas exchange, decreased lung compliance, and increased work of breathing. While it may be associated with ineffective airway clearance, it is not as specific as a weak, nonproductive cough for indicating this particular problem.
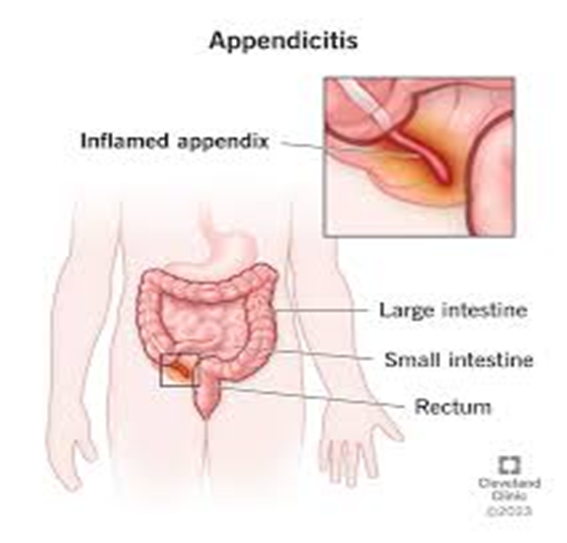
A client with suspected appendicitis is awaiting surgery. What action should the nurse take?
Explanation
Choice A reason:
Offering a warm beverage to a client with suspected appendicitis is not advisable. Preoperative clients are typically required to have an empty stomach to reduce the risk of aspiration during anesthesia. Introducing fluids or food could delay surgery and increase the risk of complications.
Choice B reason:
Monitoring the client's gag reflex is not a priority in the care of a client with suspected appendicitis. The gag reflex is more relevant in neurological assessments or when evaluating swallowing function, not in the context of appendicitis.
Choice C reason:
Helping the client to a side-lying position with knees flexed can provide comfort and may help relieve abdominal pain. This position reduces tension on the abdominal muscles and can be a supportive measure while the client awaits surgery.
Choice D reason:
Applying a heating pad to the abdomen is contraindicated in clients with suspected appendicitis. Heat can cause the appendix to rupture, leading to peritonitis, which is a severe and potentially life-threatening complication. Therefore, this action should be avoided.
How can the nurse assess that the outcomes of nursing interventions have been successful for a client diagnosed with a sickle cell crisis? (SELECT ALL THAT APPLY)
Explanation
Choice A reason:
Being free of chest pain and dyspnea is a significant indicator of successful nursing intervention in a sickle cell crisis. Chest pain and dyspnea can occur due to acute chest syndrome, a life-threatening complication of sickle cell disease characterized by vaso-occlusion in the pulmonary microcirculation. Effective pain management and oxygen therapy can alleviate these symptoms, reflecting improved respiratory function and gas exchange.
Choice B reason:
Educating the client on the importance of increasing fluid intake is crucial in managing sickle cell crisis. Adequate hydration helps to reduce blood viscosity and prevent sickling of red blood cells, which can lead to vaso-occlusive episodes. When a client verbalizes understanding and the importance of hydration, it demonstrates the effectiveness of patient education and the client's engagement in self-care.
Choice C reason:
While increasing aerobic exercises may promote endurance, it is not typically a short-term outcome measure for a sickle cell crisis. Exercise must be approached with caution in these clients, as it can increase the risk of a vaso-occlusive crisis due to dehydration and increased oxygen demand during a sickle cell crisis.
Choice D reason:
Control of acute pain to a level of 3 on a standard pain scale indicates successful pain management, a primary goal in the treatment of sickle cell crisis. Pain in sickle cell crisis is due to ischemia from obstructed blood flow by sickled cells. Effective analgesic administration and pain management strategies are essential to achieve this outcome.
Choice E reason:
A leukocyte count of 18,000/mm³ is above the normal range (4,500 to 11,000/mm³) and may indicate an infection or inflammation, which are common complications of sickle cell disease. However, this is not a direct outcome of nursing interventions aimed at managing a sickle cell crisis and thus is not a correct choice.
The nurse is conducting discharge teaching for a client with Type 2 diabetes who is on insulin glargine. The nurse knows the teaching has been effective when the client states:
Explanation
Choice A reason:
This statement is incorrect. Insulin glargine is a long-acting insulin with a relatively steady effect and does not require eating within a specific timeframe after injection. It is designed to be injected once daily at any time of the day but at the same time every day.
Choice B reason:
This statement is incorrect. Insulin glargine should not be mixed with any other insulins in the same syringe. It is formulated to be clear and colorless, and mixing it with other insulins, especially rapid-acting insulins like lispro, can affect its action profile.
Choice C reason:
This statement is correct. Rotating the injection site is important to prevent lipodystrophy, which is the breakdown or buildup of fat beneath the skin that can occur with repeated injections at the same site. Rotating sites helps to ensure consistent insulin absorption.
Choice D reason:
This statement is correct. Insulin glargine should be administered in areas of subcutaneous fat, such as the upper arms, thighs, buttocks, or abdomen. The upper anterior aspect of the arm is an appropriate site for insulin injection.
After examining and treating a client who has been raped, what discharge instructions should be provided by the emergency department (ED)?
Explanation
Choice A reason:
Providing information about available community resources is crucial for ongoing support and assistance. These resources can offer counseling, medical follow-up, legal advice, and other services that may be needed after such a traumatic event. Community resources play a vital role in the recovery process, offering a network of support and specialized services tailored to the needs of sexual assault survivors.
Choice B reason:
While it is important to know when to return to the ED for follow-up care, this is typically not the primary content of discharge instructions. Follow-up care is usually managed by primary care providers or specialists rather than the ED unless there are specific complications or concerns that need to be addressed immediately.
Choice C reason:
The names and phone numbers of local attorneys may be provided, but this is not standard for all discharge instructions. Legal support is important, but the immediate focus post-discharge is often on the survivor's physical and emotional well-being. Attorneys specializing in defending rape victims can be a part of the community resources provided to the survivor.
Choice D reason:
The phone number of a battered women's shelter or safe house may be included in discharge instructions, especially if there is an immediate need for safe accommodation. However, this is not the only resource that should be provided, and it is not specific to all cases of sexual assault.
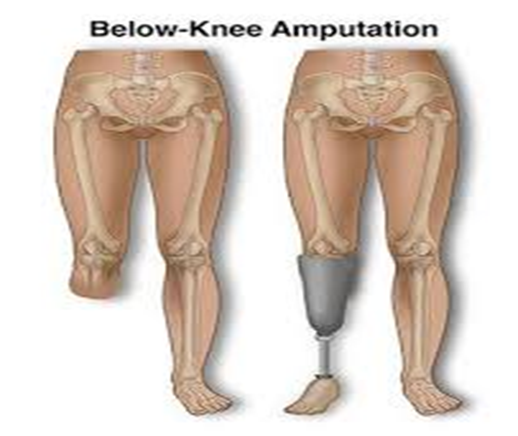
What nursing action(s) should be included in the post-op care plan for a client recovering from a below-the-knee amputation?
Explanation
Choice A reason:
Post-operative pain management is a critical aspect of care for a client recovering from a below-the-knee amputation. Administering pain medication as needed helps to manage pain effectively, which is essential for the client's comfort and recovery. Pain control is also important to facilitate participation in rehabilitation activities.
Choice B reason:
It is not advisable to encourage the client to bear weight on the affected limb immediately after surgery. The residual limb needs time to heal, and premature weight-bearing can lead to complications such as delayed healing or wound dehiscence.
Choice C reason:
While it is important to prevent complications such as deep vein thrombosis, complete restriction of mobility and keeping the client on bed rest is not recommended. Early mobilization, as part of a rehabilitation program, is essential for improving circulation, preventing muscle atrophy, and promoting overall recovery.
Choice D reason:
Applying a tight compression bandage on the residual limb is a common practice in the post-operative care of clients with amputations. The compression bandage helps to control swelling, shape the limb for a prosthesis, and prevent fluid accumulation. However, the bandage must be applied correctly to avoid impairing circulation.
The nurse is sitting with a client diagnosed with schizophrenia who suddenly begins laughing uncontrollably, even though nothing humorous has been said. The nurse should respond by saying:
Explanation
Choice A Reason:
Asking the client to share the joke may imply that the nurse believes the client is laughing at a joke, which may not be the case. It's important to recognize that uncontrollable laughter can be a symptom of schizophrenia and not necessarily a response to humor.
Choice B Reason:
This response is open-ended and nonjudgmental, inviting the client to explain their behavior without making assumptions. It allows the client to share their experience, which could be related to an internal stimulus such as a hallucination or simply a response they cannot control.
Choice C Reason:
Asking "Why are you laughing?" could be perceived as confrontational or accusatory. It might make the client feel defensive or misunderstood, especially if the laughter is a symptom of their condition and not something they are doing voluntarily.
Choice D Reason:
Saying "I don't think I said anything funny" focuses on the nurse's perspective rather than the client's experience. It could inadvertently dismiss the client's behavior as inappropriate or unjustified, which is not supportive in a therapeutic relationship.
A client diagnosed with depression prefers alternative therapy instead of prescription medication. Which alternative therapy has been proven effective in treating this condition?
Explanation
Choice A Reason:
St. John's Wort is a well-known herbal remedy that has been used for centuries to treat various ailments, including depression. It is believed to work by increasing the levels of neurotransmitters in the brain, such as serotonin, which can help improve mood and alleviate depressive symptoms. Clinical studies have shown that St. John's Wort can be effective for mild to moderate depression.
Choice B Reason:
Black Cohosh is primarily used to relieve symptoms associated with menopause, such as hot flashes and night sweats. While it may have some mood-stabilizing effects, there is insufficient evidence to support its use as a primary treatment for depression.
Choice C Reason:
Peppermint is commonly used for its soothing properties to aid digestion and reduce headaches. However, it is not typically used as a treatment for depression, and there is no substantial evidence to suggest it would be effective for this purpose.
Choice D Reason:
Echinacea is best known for its potential to boost the immune system and reduce symptoms of colds and other infections. It is not recognized as a treatment for depression, and there is no significant research to support its use in this context.
A nurse is evaluating a client who has been on prednisone after an exacerbation of inflammatory bowel disease. Which finding should the nurse identify as the priority? The client reports:
Explanation
Choice A Reason:
A blood glucose level of 80 mg/dL before eating falls within the normal fasting blood glucose range, which is between 70 mg/dL to 110 mg/dL. Therefore, this finding is not a priority concern for a client taking prednisone.
Choice B Reason:
Gaining 5 pounds over 7 months is not typically a priority concern unless it is sudden or unexplained. Prednisone can cause fluid retention and weight gain as a common side effect, but this gradual weight change does not indicate an immediate health risk.
Choice C Reason:
Waking up with a fever is a priority finding as it may indicate an infection. Patients on prednisone are at increased risk of infections due to its immunosuppressive effects¹. Fever could also signify an exacerbation of inflammatory bowel disease or other complications.
Choice D Reason:
While insomnia is a common side effect of prednisone and can impact quality of life, it is not typically a priority over signs that could indicate infection or exacerbation of the underlying condition
The nurse is reviewing pre-operative lab results for an adult client on a medical-surgical unit. Which finding should be reported to the physician immediately?
Explanation
Choice A Reason:
Sodium levels in the blood should normally be between 135 and 145 mEq/L. A level of 152 mEq/L is considered high and can be indicative of hypernatremia, which requires prompt medical attention to address potential dehydration, kidney issues, or other underlying conditions.
Choice B Reason:
Potassium levels should be within the range of 3.5 to 5.2 mEq/L for adults. A result of 3.8 mEq/L falls within the normal range, indicating no immediate concern regarding potassium levels.
Choice C Reason:
Calcium levels in the blood are typically between 8.6 and 10.2 mg/dL for adults. Therefore, a calcium level of 10.0 mg/dL is within the normal range and does not require urgent reporting to a physician.
Choice D Reason:
Creatinine levels in the blood should be between 0.6 to 1.3 mg/dL in adults, depending on factors such as age, gender, and muscle mass. A level of 1.2 mg/dL is at the higher end of the normal range but is not typically considered critical unless there are other signs of kidney dysfunction.
A 40-year-old client reports chronic lower back pain and stiffness. X-rays of the lumbar spine confirm a diagnosis of moderate to severe osteoarthritis. The nurse identifies which predisposing factor might have contributed to these degenerative changes?
Explanation
Choice A Reason:
Weekly aerobic exercise at a gym is generally beneficial for joint health and is not a predisposing factor for osteoarthritis. Regular physical activity helps maintain joint flexibility, muscle strength, and overall health, which can actually help prevent the development of osteoarthritis.
Choice B Reason:
Vitamin D deficiency has been associated with an increased risk of osteoarthritis. Vitamin D is essential for bone health, and a deficiency can lead to changes in bone structure and strength, potentially contributing to the development and progression of osteoarthritis.
Choice C Reason:
A weight of less than 60 kg does not typically predispose an individual to osteoarthritis. In fact, maintaining a healthy weight can reduce the risk of developing osteoarthritis, as excess body weight can increase the stress on joints.
Choice D Reason:
Trauma can lead to post-traumatic osteoarthritis, which is a form of osteoarthritis that develops after an injury to a joint. Traumatic injuries can damage the cartilage and bone, leading to degenerative changes and osteoarthritis.
Sign Up or Login to view all the 92 Questions on this Exam
Join over 100,000+ nursing students using Nursingprepexams’s science-backend flashcards, practice tests and expert solutions to improve their grades and reach their goals.
Sign Up Now

