Mental Health Chapter 1 - Exam 2
Total Questions : 41
Showing 25 questions, Sign in for moreA long-term goal for in patient mental health treatment is generally to:
Explanation
The ultimate goal of inpatient mental health treatment is to help patients stabilize and manage their mental illness to the point where they can safely return to their homes and communities. Inpatient treatment is typically only used for short periods of time to stabilize a patient who is experiencing severe symptoms that cannot be managed on an outpatient basis. Once the patient is stabilized, they can be discharged and transitioned to an outpatient treatment program or a community mental health centre.
While some mental illnesses may be curable, many are chronic conditions that require ongoing management and treatment.
Finding a facility for long-term care may be appropriate in some cases, but it is not generally a goal of inpatient mental health treatment.
Being arrested and placed in prison is not a desirable outcome of mental health treatment and is not a goal of the treatment process.
A breakthrough of the 1950s that assisted in the deinstitutionalization movement was:
Explanation
The development of psychotropic medications in the 1950s was a major breakthrough that helped to facilitate the deinstitutionalization movement. These medications helped to manage the symptoms of mental illness and allowed many patients to be treated in community-based settings rather than being confined to institutions. This shift towards community-based care was further supported by the Community Mental Health Centers Act and other initiatives.
A nurse is working with a patient and atempts to communicate effectively with him or her. Techniques the nurse can use to help communication include: (Select all that apply)
Explanation
These techniques can help a nurse communicate effectively with a patient. Clarifying terms can help ensure that both the nurse and the patient understand each other and are on the same page.
Remaining silent can give the patient space to express themselves and can show that the nurse is actively listening.
Asking open-minded questions can encourage the patient to share their thoughts and feelings and can help the nurse beter understand the patient’s perspective.
Offering false reassurance and discouraging the person from expressing feelings that are unacceptable (e) are not effective communication techniques. False reassurance can undermine trust and discourage honest communication, while discouraging expression of feelings can prevent the patient from fully engaging in the therapeutic process.

Nurses who care for patients who are homeless understand that the in the United States:
Explanation
Nurses who care for patients who are homeless understand that homelessness is a complex issue and that there are many factors that can contribute to it. While mental illness can be a contributing factor, it is not the only one and not all homeless individuals have a mental illness. It is important for nurses to approach each patient as an individual and to provide care that is tailored to their specific needs and circumstances.

A client can be involuntarily admitted to a psychiatric facility for the following reasons: (Select all that apply)
Explanation
Involuntary admission to a psychiatric facility, also known as involuntary commitment, is a legal process in which a person is admitted to a psychiatric hospital without their consent. The criteria for involuntary admission may vary depending on the jurisdiction, but generally include a determination that the person is a danger to themselves or others or is unable to care for themselves due to a mental illness.
Therefore,
Options b, c, and d are all valid reasons for involuntary admission, as they relate to the person's ability to cause harm to themselves or others or their inability to care for themselves.
Options a and e, on the other hand, are not valid reasons for involuntary admission as they do not relate to the person's mental state or potential for harm to themselves or others.
Which nursing theorists promoted the interpersonal theory between patient and nurse?
Explanation
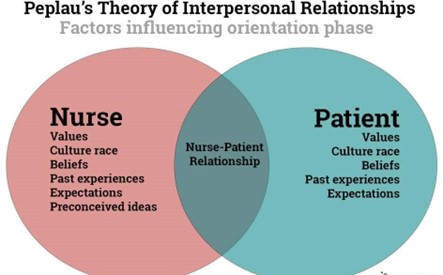
Hildegard Peplau was a nursing theorist who promoted the interpersonal theory between patient and nurse. She believed that nursing is a therapeutic, interpersonal process that involves the development of a close and personal relationship between the nurse and the patient. According to her theory, the nurse should understand the patient's needs, feelings, and behaviors to develop a personalized care plan that would facilitate the patient's recovery.
Mary Mahoney was a nurse who broke racial barriers and became the first African American registered nurse in the United States.
Hattie Bessment was a nurse who promoted nursing education and research.
Linda Richards was the first professionally trained nurse in the United States and established the first nursing school in Japan.
While these nurses contributed significantly to the nursing profession, they did not specifically promote the interpersonal theory between patient and nurse.
Linda is pacing the floor and appears extremely anxious. The daily shift nurse approaches Linda to lessen her anxiety. The most therapeutic statement by the nurse would be:
Explanation
This statement shows that the nurse is interested in Linda's feelings and is willing to listen to her. It allows Linda to express her emotions and concerns, which can help to reduce her anxiety.
Option A ("How about watching a football game?") may not be appropriate as Linda may not be interested in football or may not find it helpful in reducing her anxiety.
Option B ("What do you have to be upset about now?") is not a therapeutic statement as it can be perceived as dismissive and invalidating of Linda's feelings.
Option D ("Ignore the client.") is never an appropriate approach for a nurse or any healthcare professional as it goes against the principles of providing care and support to patients.

The following types of patients require adaptive communication techniques: (Select all that apply)
Explanation
These patients may require adaptive communication techniques to help them communicate effectively with their healthcare providers. For example, a patient with dysphasia may benefit from the use of visual aids or gestures to help them understand and express themselves. A patient who is deaf may require the use of sign language or other forms of non-verbal communication. A patient who is blind may benefit from the use of tactile or auditory aids to help them communicate.
While patients who have schizophrenia (b) or are elderly (c) may also have communication challenges, these conditions do not necessarily require the use of adaptive communication techniques. It is important for healthcare providers to assess each patient’s individual needs and to provide appropriate support and accommodations to help them communicate effectively.
Which question asked by the nurse would gain the most information from a patient experiencing marital crisis?
Explanation
This open-ended question allows the patient to share their thoughts and feelings about their relationship and provides the nurse with valuable information about the patient’s situation. By asking this question, the nurse is showing that they are actively listening to the patient and are interested in understanding their perspective.
The other questions (b, c, d) are more closed-ended and may not provide as much information about the patient’s situation. It is important for the nurse to ask open-ended questions and to actively listen to the patient’s responses to gain a better understanding of their needs and concerns.
The nurse in the Emergency Department finds a woman collapsed on the floor and crying loudly. The woman’s husband was in a car accident and is being attended by the medical staff.
Which statement by the medical nurse best demonstrates acting in a culturally competent manner?
Explanation
In this situation, the nurse is recognizing that the woman is distressed and is showing empathy and understanding by offering her a private space to talk. This allows the woman to express herself freely without feeling judged or embarrassed in front of others. It also shows the nurse's respect for the woman's privacy and her cultural beliefs, which may include the need for modesty and privacy during emotional situations.
Option A is not culturally competent because it dismisses the woman's emotional state and implies that her behavior is abnormal.
Option B assumes that medication is the solution to the woman's emotional distress and does not address her cultural needs.
Option C is not culturally competent because it disregards the woman's feelings and emotions and implies that her reaction is inappropriate.
Overall, cultural competence is about being respectful and sensitive to the beliefs, values, and customs of individuals and communities from diverse backgrounds, and providing care that is tailored to their unique needs and preferences.
A nurse tells a client that she will be back in 10 minutes to re-assess the client’s pain. When the nurse returns in 10 minutes, which aspect of the therapeutic relationship is the nurse developing?
Explanation
Trust is an essential component of a therapeutic relationship between a healthcare provider and a patient. By promising to return and re-assess the client's pain in a timely manner, the nurse is demonstrating reliability and follow-through, which can help to build trust between the nurse and the client.
Option c is therefore the correct answer.
Sympathy refers to feeling sorry for someone's situation or emotions.
Empathy is the ability to understand and share the feelings of another person.
Closure refers to the process of ending a therapeutic relationship in a way that is satisfactory for both the patient and the healthcare provider. None of these options accurately describes the aspect of the therapeutic relationship that the nurse is developing in this scenario.
A nurse is interacting with a client who is expressing her feelings about her child’s insensitive behavior. Which statement made by the nurse indicates the nurse is empathizing with the client?
Choose the best answer.
Explanation
Empathy is the ability to understand and share the feelings of another person. It involves acknowledging and validating the other person's emotions and experiences. In this scenario, the nurse should demonstrate empathy towards the client who is expressing her feelings about her child's insensitive behavior.
Option a is dismissive and minimizes the client's concerns. It does not show empathy or understanding of the client's situation.
Option b might sound sympathetic, but it could also come across as pitying, which may not be helpful or supportive for the client. It also does not reflect an understanding of the client's feelings.
Option d is judgmental and critical, and it could make the client feel defensive and unsupported.
Option c is the best response as it shows empathy and validates the client's emotions. It acknowledges the client's difficulty and demonstrates the nurse's understanding and support for the client's situation.
Which nurse responses could block effective communication with a client?
(Select all that apply)
Explanation
Why did you do that? - This question can come across as judgmental and accusatory, and may cause the client to become defensive or feel criticized.
Tell me more about your relationship with your daughter? - This question encourages the client to open up and share more about themselves, which can promote effective communication.
This is what I think you should say. - This response takes away the client's autonomy and can make them feel like their feelings and opinions are not important.
Don’t stress over it, everything will turn out fine. - This response minimizes the client's concerns and can make them feel like their feelings are not valid or important. It can also come across as dismissive and unempathetic.
A female client tells the nurse that she feels very depressed about her recent divorce. Which of the following is the nurses best therapeutic response?
Explanation
This response is empathetic and allows the client to express her feelings openly. It demonstrates active listening and validates the client's emotions.
Option A ("I know exactly how you feel") can come across as dismissive or assuming, and it may not accurately reflect the client's unique experience.
Option B ("Most people experience depressed feelings after a divorce") may also come across as dismissive and minimizes the client's feelings.
Option C ("Look on the bright side, you will be glad you divorced him in a couple of years") is not empathetic and does not acknowledge the client's current emotional state.
While dining in a restaurant the nurse overhears two co-workers in the next booth discussing a client who is being cared for on the mental health unit which they work.
What action have the nurse’s co-workers committed for which they could be held liable for?
Explanation
Breach of confidentiality occurs when private and sensitive information is disclosed to others without the client's consent. In this scenario, the co-workers are discussing a client's mental health condition in a public place where their conversation can be overheard by others. This is a violation of the client's right to privacy and confidentiality.
The co-workers could be held liable for breaching the client's confidentiality and may face disciplinary action or legal consequences. It is important for healthcare providers to maintain confidentiality to protect their clients' privacy and trust.

While the nurse is talking with a female client, the client becomes quiet for several hours. Which is the nurse’s best response?
Explanation
a. To maintain silence and be attentive to the client’s nonverbal communication and let the client gather his/her thoughts.
The best response for the nurse in this situation is to maintain silence and be attentive to the client's nonverbal communication. This allows the client to gather her thoughts and continue the conversation when she is ready. Interrupting the silence with a question or trying to push the client to share her feelings may cause her to withdraw further. It is important for the nurse to respect the client's pace and provide a safe and supportive environment for her to express her thoughts and feelings. Therefore,
Option a is the correct answer.
A nurse is caring for a client on an acute care mental health unit who was involuntarily admitted for 72 hr. after attacking a neighbor.
To keep the client in the hospital when the initial time to hold the client expires, which of the following must be determined?
Explanation
Involuntary admission to a mental health unit is done when an individual poses a threat to themselves or others due to a mental health condition. The initial hold is usually for 72 hours, during which the client's condition is assessed and an appropriate treatment plan is developed. If the client is still deemed to be a danger to themselves or others after the initial hold, the healthcare provider may request an extension of the hold or seek a court order to continue treatment.
In order to keep the client in the hospital, it must be determined that they continue to pose a threat to themselves or others.
Factors such as the client's ability to make arrangements to stay with someone or financial capability to pay for medications are not relevant to the decision of whether to continue the hold.
Similarly, unwillingness to accept treatment is not the determining factor, as involuntary treatment can be provided to clients who do not recognize their need for treatment if they are deemed to be a danger to themselves or others.
The nursing student is assigned a client to interview and is asked to practice the therapeutic communication techniques of stating the implied and making and observation about their behavior.
Which statement by the student nurse best describes the technique?
Explanation
This statement by the student nurse demonstrates the technique of stating the implied and seeing the client's behavior. The student nurse has observed the client pacing the halls and having a tense look on their face, which implies that the client may be feeling anxious. By stating this observation to the client, the student nurse is validating the client's experience and opening a dialogue about their feelings. This technique can help the client feel heard and understood and can facilitate a therapeutic relationship between the client and the nurse.
Option B is an open-ended question that can encourage the client to share more about their feelings, but it does not demonstrate the technique of stating the implied and making an observation about the client's behavior.
Option C is a statement that may be perceived as judgmental or confrontational and does not demonstrate the technique of stating the implied and making an observation about the client's behavior.
Option D is a statement that is focused on the nurse's agenda rather than the client's needs and does not demonstrate the technique of stating the implied and seeing the client's behavior.
An order written by the physician is reviewed by the nursing staff, and no one is familiar with the treatment instructions. A nurse who is recently hired knows that this treatment is covered by the states nurse practice act.
What is the nurses’ best course of action?
Explanation
When faced with an unfamiliar treatment instruction, it is important for the nurse to consult the facility’s policies and procedures to determine the appropriate course of action. These policies and procedures provide guidance on how to carry out treatments safely and effectively and can help ensure that the patient receives the best possible care.
While it may also be appropriate for the nurse to call the physician for clarification (a), check the state’s nurse practice act (b), or contact the nursing supervisor for approval (d), consulting the facility’s policies and procedures should be the first step in determining the appropriate course of action.
The nurse’s ability to use therapeutic communication effectively in the mental health setting depends on:
Explanation
The nurse’s ability to listen and observe the client’s verbal and non-verbal messages. Effective communication in the mental health setting requires the nurse to actively listen to the client and to pay close attention to their verbal and non-verbal cues. By doing so, the nurse can better understand the client’s needs and concerns and can provide appropriate support and guidance.
While the nurse’s understanding of mental health disorders (b) and their relationship with the client (d) can also play a role in effective communication, the ability to listen and observe is a fundamental skill that is essential for effective therapeutic communication. The client’s ability to communicate (a) is also important, but it is ultimately the nurse’s responsibility to use effective communication techniques to facilitate the therapeutic process.
An example of a client who requires emergency admission to a mental hospital is one who has been diagnosed with:
Explanation
This client’s behavior indicates that they may pose a danger to themselves or others and may require immediate intervention to ensure their safety and the safety of those around them.
The other clients (a, b, c) may also have mental health needs, but their situations do not necessarily indicate the need for emergency admission to a mental hospital. It is important for healthcare providers to assess each client’s individual needs and to provide appropriate care and support.
While working as nurse in a hospital you notice that a co-worker has unsteady gait and slurred speech. You suspect that she may be an impaired nurse.
Which of the following will be the appropriate action to take?
Explanation
This is because impaired nursing can have serious consequences for patients' safety and well-being, and it is your ethical and professional responsibility to take action to ensure patient safety.
Confronting the co-worker directly ( Option d) may not be the best approach, as it could lead to a confrontational situation and may not resolve the issue. Asking your co-worker to perform a sobriety test ( Option a) may also not be appropriate, as you may not be trained or authorized to administer such a test, and it may not be a reliable indicator of impairment. Ignoring the co-worker's behavior ( Option c) is not an appropriate action, as it could potentially harm patients and violate your ethical and professional responsibilities as a nurse.
During a client nurse interaction, which nursing statement may give the client false reassurance?
Explanation
This statement may give the client false reassurance because it dismisses the client's concerns without acknowledging or addressing them. It is important for the nurse to listen to the client's concerns and provide appropriate interventions and support rather than simply dismissing their worries with a blanket statement. The other
Options (a, b, and c) are observations of the client's behavior or appearance, and do not provide false reassurance.
The capacity to understand or feel what another person is experiencing from within the other persons frame of reference i.e., the capacity to place oneself in another person’s position:
Explanation
Empathy is the capacity to understand or feel what another person is experiencing from within the other person's frame of reference. It involves recognizing and sharing the emotions and perspectives of others, without necessarily experiencing the same emotions or perspectives oneself.
Telepathy, on the other hand, refers to the supposed ability to communicate with others through thoughts or mental processes, without the use of normal sensory channels such as sight or sound.
Sympathy refers to feelings of pity or sorrow for someone else's misfortune. It involves feeling sorry for someone, but not necessarily understanding or sharing their perspective.
Apathy refers to a lack of interest or concern and can be seen as the opposite of empathy.
The set of rules designed to protect patients who are described as vulnerable are known as?
Explanation
The Patients’ bill of rights is a set of rules that protect patients and ensure that they are treated with dignity, respect, and autonomy. It describes the rights that patients have when they receive medical care and treatment. The Patients’ bill of rights was created to protect patients who are vulnerable and may not have the ability or resources to advocate for themselves.
The Doctrine of privileged information refers to the legal concept that certain information shared between a patient and healthcare provider is confidential and cannot be disclosed without the patient’s consent.
Collaborative practice refers to the coordinated efforts of healthcare professionals from different disciplines working together to provide comprehensive and high-quality patient care.
The Nurse practice act is a set of laws that govern the practice of nursing in a specific state or jurisdiction. It outlines the scope of nursing practice and the responsibilities and obligations of nurses.

Sign Up or Login to view all the 41 Questions on this Exam
Join over 100,000+ nursing students using Nursingprepexams’s science-backend flashcards, practice tests and expert solutions to improve their grades and reach their goals.
Sign Up Now

