Immediate Newborn Care > Maternal & Newborn
Exam Review
More questions on this topic
Total Questions : 16
Showing 16 questions, Sign in for moreA nurse is assessing a newborn’s vital signs at 1 hour of age.
Which of the following findings should the nurse report to the provider?
Explanation
The correct answer is choice C. A temperature of 36°C (96.8°F) is below the normal range for a newborn, which is 36.5°C to 37.5°C (97.7°F to 99.5°F).
A low temperature can indicate hypothermia, infection, or hypoglycemia, and should be reported to the provider.
Choice A is wrong because a heart rate of 140/min is within the normal range for a newborn, which is 120 to 160/min.
Choice B is wrong because a respiratory rate of 50/min is within the normal range for a newborn, which is 30 to 60/min.
Choice D is wrong because a blood pressure of 60/40 mm Hg is within the normal range for a newborn, which is 50 to 75/30 to 45 mm Hg.
A nurse is preparing to administer hepatitis B vaccine to a newborn whose mother is hepatitis B surface antigen negative (HBsAg-).
Which of the following actions should the nurse take?
Explanation
The correct answer is choice B. Give the vaccine intramuscularly in the anterolateral thigh.
This is because the anterolateral thigh is the recommended site for intramuscular injections in infants less than 12 months of age.
It has a large muscle mass and minimal risk of injury to nerves or blood vessels.
Choice A is wrong because informed consent is not required for routine immunizations, unless the parent or guardian requests more information or declines the vaccine.
Choice C is wrong because hepatitis B immune globulin (HBIG) is only indicated for newborns whose mothers are hepatitis B surface antigen positive (HBsAg+), as they have a high risk of acquiring the infection from their mothers.
Choice D is wrong because there is no need to delay giving the vaccine until after breastfeeding is established.
Breastfeeding does not interfere with the vaccine’s effectiveness or safety, and it does not increase the risk of adverse reactions.
A nurse is performing an initial assessment of a newborn who was delivered vaginally at term with no complications.
Which of the following findings should alert the nurse to a potential problem?
Explanation
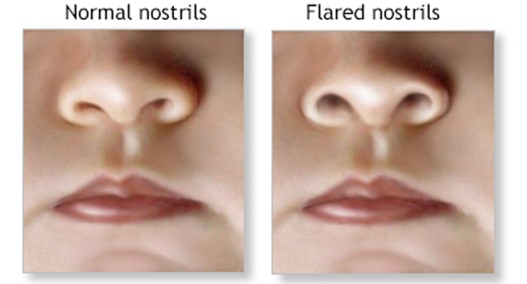
The correct answer is choice C. Nasal flaring and grunting are signs of respiratory distress in a newborn and should alert the nurse to a potential problem.
The nurse should monitor the newborn’s respiratory rate, oxygen saturation, and chest movements, and notify the provider if the symptoms persist or worsen.
Choice A is wrong because molding of the head is a normal finding in a newborn who was delivered vaginally.
It is caused by the pressure of the birth canal on the skull bones and usually resolves within a few days.
Choice B is wrong because acrocyanosis of hands and feet is a normal finding in a newborn during the first 24 hours of life.
It is caused by poor peripheral circulation and does not indicate hypoxia or cyanosis.
Choice D is wrong because vernix caseosa on skin folds is a normal finding in a newborn.
It is a white, cheesy substance that protects the skin from amniotic fluid and helps with thermoregulation.
It usually disappears within a few days.
A nurse is caring for a newborn who has received erythromycin eye ointment as prophylaxis for ophthalmia neonatorum.
What should the nurse monitor for as a potential adverse reaction to this medication?
Explanation
The correct answer is choice A. Hypersensitivity.Erythromycin eye ointment is an antibiotic that can cause allergic reactions in some newborns, such as irritation, redness, swelling, or cloudy eyes.
This is a potential adverse reaction to this medication that the nurse should monitor for.
Choice B. Glaucoma is wrong because glaucoma is a condition that causes increased pressure in the eye and can damage the optic nerve.
It is not caused by erythromycin eye ointment.
Choice C. Cataracts is wrong because cataracts are a condition that causes clouding of the lens of the eye and can impair vision.
It is not caused by erythromycin eye ointment.
Choice D. Strabismus is wrong because strabismus is a condition that causes misalignment of the eyes and can affect depth perception.
It is not caused by erythromycin eye ointment.
Erythromycin eye ointment is used to prevent ophthalmia neonatorum, which is an infection of the eye surface that affects newborns within the first month of life.It can be caused by bacteria such as chlamydia or gonorrhea that can enter the baby’s eyes during childbirth and cause permanent damage to the corneas.Erythromycin eye ointment can help prevent vision loss caused by these bacteria.
A nurse is administering erythromycin eye ointment to a newborn who has a history of allergic reaction to penicillin.
What should the nurse do before applying the ointment?
Explanation
The correct answer is choice B. Check if there is any cross-sensitivity between erythromycin and penicillin.Erythromycin is a macrolide antibiotic that can be used to treat bacterial eye infections in newborns and adults.
Penicillin is a beta-lactam antibiotic that can cause allergic reactions in some people.
Cross-sensitivity means that a person who is allergic to one type of antibiotic may also be allergic to another type of antibiotic that has a similar structure or mechanism of action.Erythromycin and penicillin have different structures and mechanisms of action, but there is still a small chance of cross-sensitivity between them.
Therefore, the nurse should check if the newborn has any history of allergic reaction to penicillin before applying the erythromycin eye ointment.
Choice A is wrong because asking the mother if she has any allergies to antibiotics is not enough to determine if the newborn is at risk of an allergic reaction to erythromycin.
The newborn may have inherited or developed an allergy to penicillin or erythromycin that the mother does not have.
Choice C is wrong because applying a small amount of ointment on the skin to test for allergic reaction is not a reliable method to diagnose an allergy.Skin testing can cause false positive or false negative results, and it may also trigger a severe allergic reaction in some cases.
Choice D is wrong because administering an antihistamine to prevent anaphylaxis is not appropriate for a newborn who has not been exposed to the allergen yet.
An antihistamine is a medication that blocks the effects of histamine, a chemical that causes allergic symptoms.
Anaphylaxis is a life-threatening allergic reaction that involves multiple organ systems and requires immediate medical attention.An antihistamine cannot prevent anaphylaxis, and it may also cause side effects such as drowsiness, dry mouth, or low blood pressure in a newborn.
A nurse is reviewing laboratory results for a newborn who received vitamin K injection at birth.
Which of the following coagulation factors should be activated by vitamin K?
Explanation
The correct answer is choice A.Factor II, also known as prothrombin, is one of the coagulation factors that are activated by vitamin K.Vitamin K is a cofactor for the carboxylation of specific glutamic acid groups in coagulation factors II, VII, IX, and X.
This process is essential for the activation of these factors in the coagulation cascade.
Choice B is wrong because factor V is not a vitamin K-dependent coagulation factor.
Factor V is activated by thrombin and acts as a cofactor for factor Xa in the conversion of prothrombin to thrombin.
Choice C is wrong because factor VIII is not a vitamin K-dependent coagulation factor.
Factor VIII is activated by thrombin and acts as a cofactor for factor IXa in the activation of factor X.
Choice D is wrong because factor XI is not a vitamin K-dependent coagulation factor.
Factor XI is activated by factor XIIa and activates factor IX in the intrinsic pathway of coagulation.
Normal ranges for coagulation factors are:
• Factor II: 70-120% of normal activity
• Factor V: 50-150% of normal activity
• Factor VIII: 50-150% of normal activity
• Factor IX: 50-150% of normal activity
• Factor X: 70-140% of normal activity
• Factor XI: 70-150% of normal activity
A nurse is caring for a newborn who has early-onset VKDB due to maternal use of anticoagulants during pregnancy.
Which of the following interventions should the nurse anticipate for this newborn?
Explanation
The correct answer is choice A. Administer fresh frozen plasma.This is because fresh frozen plasma contains clotting factors that can help stop the bleeding caused by vitamin K deficiency.Vitamin K is needed for the synthesis of clotting factors in the liver, but newborns have low levels of vitamin K and may develop vitamin K deficiency bleeding (VKDB) if they do not receive prophylaxis at birth.VKDB can manifest as bleeding in various sites, such as the skin, mucous membranes, umbilicus, gastrointestinal tract, or central nervous system.
Choice B is wrong because packed red blood cells do not contain clotting factors and will not correct the underlying deficiency of vitamin K.
Choice C is wrong because intravenous immunoglobulin is used to treat immune-mediated thrombocytopenia, not vitamin K deficiency.
Choice D is wrong because recombinant erythropoietin is used to stimulate red blood cell production in anemia, not to treat bleeding disorders.
Early-onset VKDB occurs within 24 hours of birth and is associated with maternal use of drugs that interfere with vitamin K metabolism, such as anticoagulants, anticonvulsants, or antituberculosis drugs.
These drugs induce the enzymes that break down vitamin K in the fetal liver
A nurse is assessing a newborn who has late-onset VKDB due to exclusive breastfeeding and inadequate oral vitamin K supplementation.
Which of the following findings should indicate a possible intracranial hemorrhage to the nurse?
Explanation
The correct answer is choice A. Bulging fontanelle.
A bulging fontanelle is a sign of increased intracranial pressure, which can be caused by intracranial hemorrhage.
Late-onset VKDB is a condition that occurs in infants who have low levels of vitamin K, which is essential for blood clotting.Most cases of late-onset VKDB present with intracranial hemorrhage.
Choice B. Sunken eyes is wrong because it is a sign of dehydration, not intracranial hemorrhage.
Choice C. Mottled skin is wrong because it is a sign of poor circulation or shock, not intracranial hemorrhage.
Choice D. Flaring nostrils is wrong because it is a sign of respiratory distress, not intracranial hemorrhage.
Normal ranges for vitamin K plasma concentrations are 0.2 to 3.2 ng/mL for adults and 0.15 to 1.5 ng/mL for infants.
A nurse is assessing a newborn who has hypoglycemia due to perinatal asphyxia.
Which of the following findings should the nurse expect? (Select all that apply.)
Explanation
The correct answer is choice A, C, D, and E.Hypoglycemia due to perinatal asphyxia can cause various neurological signs in the newborn, such as irregular respirations, apnea, eye-rolling, and lethargy.
These signs indicate inadequate oxygenation and glucose delivery to the brain.Cyanosis is not a specific sign of hypoglycemia, but rather a sign of poor oxygenation that can occur due to other causes.
Therefore, choice B is wrong.
Choice A is correct because irregular respirations can result from hypoglycemia due to perinatal asphyxia.Hypoglycemia can impair the respiratory center in the brainstem and cause irregular breathing patterns.
Choice C is correct because apnea can result from hypoglycemia due to perinatal asphyxia.
Apnea is defined as a pause in breathing
A nurse is caring for a preterm newborn who has hypoglycemia due to inadequate gluconeogenesis.
The nurse should understand that this condition occurs because preterm newborns have limited stores of which of the following substances?
Explanation
The correct answer is choice A. Glycogen.Preterm newborns have limited stores of glycogen, which is a substance made from glucose that is stored in the liver and muscle cells to be used later for energy.When blood glucose levels are low, the hormone glucagon signals the cells to convert glycogen back into glucose and release it into the bloodstream.However, preterm newborns have a reduced ability to produce glucagon and to use gluconeogenesis, which is the process of making new glucose from other sources.Therefore, they are at risk of hypoglycemia, which is a condition where blood glucose levels are too low to support normal brain function.
Choice B is wrong because glucose is the sugar that travels through the blood to fuel the cells, not a substance that is stored for later use.
Choice C is wrong because insulin is a hormone that helps cells absorb glucose from the blood, not a substance that is stored for later use.
Choice D is wrong because glucagon is a hormone that triggers the release of glucose from the liver and muscle cells, not a substance that is stored for later use.
A nurse is educating a group of college students about hepatitis B virus (HBV) transmission and prevention.
The nurse should emphasize that the most common modes of transmission are which of the following? (Select all that apply)
Explanation
The correct answer is choice A, B, C, D and E.All of these are possible modes of transmission for hepatitis B virus (HBV), which is a viral infection that attacks the liver and can cause both acute and chronic disease.The virus is most commonly transmitted from mother to child during birth and delivery, as well as through contact with blood or other body fluids during sex with an infected partner, unsafe injections or exposures to sharp instruments.
Choice A is correct because unprotected sexual contact can expose a person to the blood, semen, or vaginal fluids of an infected partner.
Choice B is correct because sharing drugs, needles, or “works” when using drugs can expose a person to the blood of an infected person.
Choice C is correct because poor infection control practices in medical settings can expose a person to contaminated needles or syringes or sharp objects that have been used on an infected person.
Choice D is correct because sharing of blood sugar (diabetes) testing equipment can expose a person to the blood of an infected person.
Choice E is correct because needle sticks or sharps exposures on the job can expose a person to the blood of an infected
A nurse is caring for a client who has chronic hepatitis B infection and is taking lamivudine (Epivir).
The nurse should monitor the client for which of the following adverse effects?
Explanation
The correct answer is choice B. Lactic acidosis.
Lamivudine (Epivir) is a nucleoside reverse transcriptase inhibitor (NRTI) used to treat chronic hepatitis B infection and HIV infection.
One of the rare but serious adverse effects of lamivudine is lactic acidosis, which is a condition where the blood becomes too acidic due to the accumulation of lactate.Lactic acidosis can cause symptoms such as nausea, vomiting, abdominal pain, muscle weakness, rapid breathing, and low blood pressure.
Choice A is wrong because pancreatitis is not a common side effect of lamivudine.
Pancreatitis is an inflammation of the pancreas that can cause severe abdominal pain, nausea, vomiting, and fever.Pancreatitis is more likely to occur with other NRTIs such as didanosine (Videx) or stavudine (Zerit).
Choice C is wrong because hypothyroidism is not a common side effect of lamivudine.
Hypothyroidism is a condition where the thyroid gland does not produce enough thyroid hormones, which regulate the metabolism and energy levels of the body.
Hypothyroidism can cause symptoms such as fatigue, weight gain, cold intolerance, dry skin, hair loss, and depression.
Hypothyroidism is more likely to occur with other drugs that interfere with thyroid function such as amiodarone (Cordarone) or lithium
A nurse is educating a new mother about umbilical cord care and how to prevent omphalitis, sepsis, and tetanus.
Which of the following statements by the mother indicates an understanding of the teaching?
Explanation
The correct answer is choice A.Washing hands before and after handling the cord stump can prevent the transmission of bacteria that can cause omphalitis, sepsis, and tetanus.
Choice B is wrong because applying petroleum jelly or ointment to the cord stump can delay its drying and increase the risk of infection.
Choice C is wrong because using hydrogen peroxide to clean the cord stump can damage the healthy tissue and delay healing.
Choice D is wrong because folding down the diaper below the cord stump can expose it to urine and feces, which can contaminate it and cause infection.
The normal range for umbilical cord separation is 5 to 15 days after birth.
A postpartum nurse instructs a new mother in how to bathe her newborn.
Which statement by the mother indicates a need for further instruction?
Explanation
The correct answer is choice B.“I should bathe him before a feeding so he won’t spit up.” This statement indicates a need for further instruction because it is not advisable to bathe a newborn infant before a feeding, as this may cause hypoglycemia or cold stress.The mother should bathe the infant after a feeding or between feedings when the infant is alert and comfortable.
Choice A is wrong because it is correct to use a clean cloth and warm water to wash around the umbilical cord.This helps prevent infection and promotes drying of the cord stump.
Choice C is wrong because it is correct to avoid getting water in the infant’s ears or eyes.This helps prevent ear infections and eye irritation.
Choice D is wrong because it is correct to dry the infant thoroughly and dress him warmly after bathing.
This helps prevent heat loss
The nurse is caring for a newborn who was circumcised using a Gomco clamp 12 hours ago and notes that there is a small amount of blood on his diaper where his penis rests against it.
The most appropriate nursing action would be to:
Explanation
The correct answer is choice C. Document this as a normal finding.According to the American Academy of Family Physicians, bleeding from the dorsal slit after circumcision using a Gomco clamp is usually minimal and will stop once the clamp is in place.
Therefore, a small amount of blood on the diaper 12 hours after the procedure is not a cause for concern and does not require any intervention.
Choice A is wrong because applying gentle pressure to stop bleeding is not necessary and may cause more trauma to the wound.
Choice B is wrong because changing the diaper more frequently may also disturb the healing process and increase the risk of infection.Choice D is wrong because notifying the physician is not indicated unless there is excessive or persistent bleeding, signs of infection, or other complications.
The nurse is teaching parents how to care for their son’s circumcision site after discharge from hospital using petroleum jelly and gauze dressing method.
Which statement by parents indicates that they need further instruction?
Explanation
The correct answer is choice B. Washing the penis with soap and water daily can irritate the circumcision site and delay healing.
The parents should only use warm water to gently clean the area and pat it dry.
They should avoid using soap, alcohol, or peroxide on the wound.
Choice A is wrong because changing the diaper every 3 to 4 hours is recommended to prevent infection and keep the area clean and dry.
Choice C is wrong because applying petroleum jelly on the penis with each diaper change can protect the wound from sticking to the diaper and reduce friction.
Choice D is wrong because calling the doctor if they see any signs of infection, such as redness, swelling, pus, foul odor, or fever, is a correct action.
Sign Up or Login to view all the 16 Questions on this Exam
Join over 100,000+ nursing students using Nursingprepexams’s science-backend flashcards, practice tests and expert solutions to improve their grades and reach their goals.
Sign Up Now

